Opioids are often prescribed for pain management after surgery — but for the 19 million people in the U.S. with a history of substance abuse, that option may not be safe or desired.
Until now, there hasn’t been a cohesive set of guidelines for managing surgical pain in patients with a history of addiction and/or opioid tolerance.
To address this, the American Society of Anesthesiologists (ASA) gathered 15 medical organizations representing over 500,000 physicians to develop seven guiding principles to improve pain management before, during and after surgery for these patients.
The guidelines have been published in the Regional Anesthesia & Pain Medicine journal.
FOR ACUTE LOWER BACK PAIN, THESE ARE THE BEST MEDICATIONS, NEW STUDY FINDS
Dr. David Dickerson, an anesthesiologist and pain specialist at North Shore University Hospital in Chicago, Illinois, is chair of the American Society of Anesthesiologists’ Committee on Pain Medicine. (ASRA is the American Society of Regional Anesthesia and Pain Medicine.)
“Patients with these complex issues may require additional care after surgery,” Dickerson told Fox News Digital.
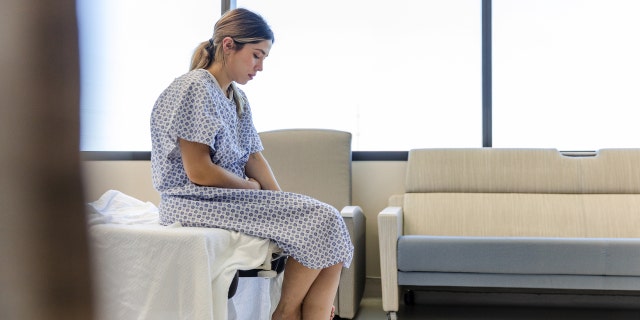
Opioids are often prescribed for pain management after surgery — but for the 19 million people in the U.S. with a history of substance abuse, that may not be a safe or desired option. Now, a new set of guidelines may help. (iStock)
“When someone undergoes a surgical procedure and they have a substance use disorder, chronic pain or pre-operative opioid tolerance, their nervous system is different,” he told Fox News Digital in an interview.
“Their ability to self-soothe in the face of injury or pain is also going to be a very different experience.”
TAKE THESE 5 SMART STEPS TO RELIEVE MUSCULOSKELETAL PAIN
As the director of four hospitals, Dickerson sees patients with many different types of pain in many different care environments. It’s why he’s calling for adopting a unified approach for patients who may not have a straightforward experience with pain management when it comes to surgery, injury, trauma or disease.
“Their ability to self-soothe in the face of injury or pain is also going to be a very different experience.”
“We want to make sure the patient has a consistent experience in terms of getting pain alleviated and also minimizing the risks of pain treatments,” he said.
Over a span of several years, Dickerson and other pain management specialists and physicians crafted the following seven principles to use as a “north star” for screening, treating and educating these vulnerable patients, while building awareness and education for safe and effective surgical care.
1. Identify patients at risk
Physicians should “screen for substance abuse preoperatively, risk stratify and refer for treatment as needed,” the first principle states.
The doctor should speak with the patient prior to surgery to determine whether there is any history of substance abuse, identify any risk factors and provide recommendations for referrals as needed.
“Clinicians should identify patients with a substance use disorder and facilitate evaluation and treatment before surgery.”
“As the majority of patients receive a post-surgery opioid prescription and 100,000 Americans die annually from accidental opioid overdose, clinicians should identify patients with a substance use disorder and facilitate evaluation and treatment before surgery,” Dickerson told Fox News Digital.
“Identifying and treating substance use disorders saves lives — especially when we recognize that 19 million Americans have at least one substance use disorder.”
2. Coordinate care for complex patients
“Coordinate care pre–operatively for complex patients and consult with pain medicine, behavioral health or addiction medicine specialists to optimize the treatment plan,” the second principle states.
This entails a multidisciplinary approach to patient care. This is when multiple health care professionals come together to define the appropriate treatment plan for an at-risk patient.

Until now, there hasn’t been a cohesive set of guidelines for managing surgical pain in patients with a history of chronic pain, addiction and/or opioid tolerance. (iStock)
“Patients with these complex issues may require additional care after surgery,” Dickerson said.
“A team of experts can plan and coordinate care that can help avoid a rocky surgical experience.”
3. Make a plan for patients already on opioids
This principle states: “For opioid-tolerant patients, coordinate and plan with the opioid prescriber to continue the home regimen; supplement analgesics perioperatively as needed.”
“Opioid-tolerant” patients are those who have been taking an opioid drug on a regular basis, resulting in the need for larger amounts to achieve the same effect.
CANCER CENTERS ARE SUFFERING MAJOR SHORTAGE OF POPULAR CHEMO DRUGS
“Patients taking opioids for weeks before surgery should not stop their opioids unless directed to do so, and clinicians should work to have a plan that avoids undertreating pain through using additional pain medications,” Dickerson said.
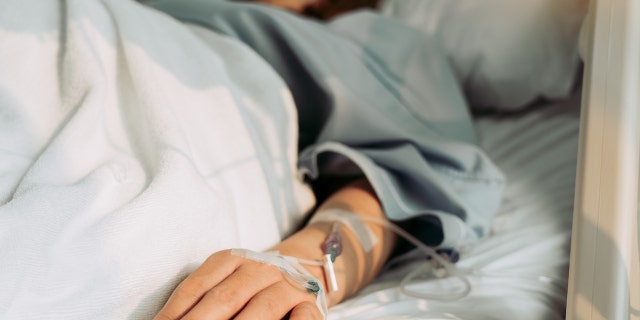
“Patients shouldn’t have to suffer after surgery with uncontrolled pain or awful medication side effects like nausea, vomiting, itching or constipation,” Dr. Dickerson said. (iStock)
In some cases, it may be necessary to continue home medications at pre-surgery doses to avoid withdrawal symptoms and a rough recovery, he noted.
“More opioids after surgery isn’t always the ideal option, either,” Dickerson added.
“There are many non-opioid therapies that are added to the home regimen to provide relief.”
4. Prescribe the lowest amount of opioids necessary
This principle states, “For opioid-tolerant patients, return to preoperative opioid dose or lower as soon as possible with an individualized tapering plan.”
In the event that an opioid-tolerant patient needs to increase the dose for post-surgery pain, the guidelines call for using the lowest necessary dose.
“Patients and their caregivers should know how to identify and respond to side effects before injury or harm occurs.”
If pre-surgery doses are increased after surgery for pain relief, those extra doses should be reduced as soon as possible as the patient heals, Dickerson said.
“This is often an individualized process, tailored to the patient’s day-to-day experience and recovery,” he added. “It is necessary to avoid creating even more significant opioid tolerance and dependence.”
5. Educate parents and caregivers
This principle says: “Educate patients and caregivers about opioid risks, how to recognize and treat respiratory depression, avoiding sedatives and alcohol, and when to call for help.”
While opioids can reduce pain, they also present specific risks and side effects that patients and their families should watch for, Dickerson said.
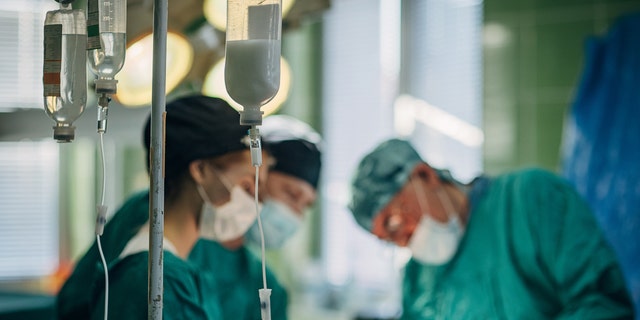
The new guidelines call for a multidisciplinary approach to patient care, in which multiple health care professionals come together to define the appropriate treatment plan for an at-risk patient. (iStock)
Additionally, he warned that alcohol and other sedatives should be avoided while taking opioids.
“Patients and their caregivers should know what to watch for and how to identify and respond to side effects before injury or harm occurs,” he said.
Some patients may be prescribed naloxone, an opioid antidote that can be given to reverse the effects of an overdose, Dickerson explained. Naloxone nasal spray can now be obtained by anyone without a prescription as an over-the-counter medication.
6. Consult with a pain specialist to provide relief as needed
“If adverse drug effects or uncontrolled pain occur, consult with a pain specialist or anesthesiologist,” this principle states.
WEIGHT LOSS SURGERIES ON THE RISE AMONG KIDS AND TEENS, STUDY FINDS: ‘ALTERING THE ANATOMY’
“Patients shouldn’t have to suffer after surgery with uncontrolled pain or awful medication side effects like nausea, vomiting, itching or constipation,” Dickerson said.
“Anesthesiologists and other pain specialists can provide additional treatments and therapies to reduce pain and the burden of side effects.”
He also said, “We have to work together to help patients have access to this team-based care.”
7. Use telehealth as needed
“If expert consultation is needed but in-person evaluation is not available, utilize telehealth to access pain medicine, behavioral health or addiction medicine,” states this principle.
Not all hospitals or clinicians have access to dedicated specialists in addiction or pain medicine, noted Dickerson. In scenarios where an in-person visit isn’t possible, the guidelines recommend relying on telehealth evaluation and consultations.

In scenarios where in-person evaluation is not available, the principles call for using telehealth to access pain medicine, behavioral health or addiction medicine. (iStock)
“We have to find a way to connect in-need patients and clinicians with help in a timely fashion and make sure patients without technology access or tech literacy still can connect with the care they need,” said Dickerson.
‘A step in the right direction’
Dr. Chris Tuell, clinical director of addiction services at the Lindner Center of HOPE at the University of Cincinnati College of Medicine, was not involved in creating the seven principles. He said he believes they are “a good start” and “a step in the right direction.”
He told Fox News Digital in an emailed statement, “We know that continuity of care and communication is essential in providing quality health care. Good treatment begins with good screening and assessment.”
“Continuity of care and communication is essential in providing quality health care.”
Given the fact that 83% of the individuals with substance use disorders also have a co-occurring mental health issue (per the Substance Abuse and Mental Health Services Administration), Tuell emphasized the need to coordinate care between the patient and his or her opioid prescriber and to create an individualized treatment plan.
“These principles stress the importance of the education of the patient and the caregiver,” he said. “Understanding the risks of opioids, and the dangers of utilizing alcohol or sedatives as a means of dealing with the adverse side effects of opioids, is essential.”
Non-opioid pain management options
In situations when someone in recovery cannot use opioids, Tuell said behavioral strategies — such as hypnotherapy, meditation and dialectical behavioral therapy — can be used to help manage pain.

Hypnotherapy is one option for non-opioid pain treatment. (iStock)
“I have utilized hypnotherapy with patients to assist in the regulation of pain when opioids were not an option,” said Tuell.
“Additionally, the use of teletherapy has provided therapy services for many underserved individuals who are residing in rural communities in which services are not readily available.”
Real patients’ stories
Dr. Lea McMahon, a licensed professional counselor, chief clinical officer at Symetria Recovery in Houston, Texas, and an adjunct professor of psychology at Columbia College, has helped many patients and people in recovery who have had to have surgery.
“From a medical viewpoint, managing pain in individuals in recovery requires an even more cautious and individualized approach,” McMahon told Fox News Digital. “These individuals often have complex needs due to the magnified effects of drug interactions, and tolerance issues.”
One patient at Symetria’s Chicago office, Ralph, 36 (he did not share his last name), became addicted to OxyContin after having surgery following a motorcycle accident in 2016.
BE WELL: TAKE THESE 5 SMART STEPS TO RELIEVE MUSCULOSKELETAL PAIN
After five years of addiction, he was in recovery for two years when he twisted his ankle in a stairwell in November 2022.
“He was already suffering a little from joint soreness before this, but he didn’t want to go back under the knife, as the pain was manageable,” said McMahon.
“However, this new injury meant he could hardly bear weight on the ankle for over a month, so he decided to have the surgery.”
Ralph had arthroscopic surgery to remove the excess scar tissue from the first operation and remove the build-up of debris.

In some cases, it may be necessary to continue home medications at pre-surgery doses to avoid withdrawal symptoms and a rough recovery, Dr. Dickerson said. (iStock)
“After a discussion with his health care provider and surgeon, it was decided to perform the operation under local general anesthetic, as with general anesthesia the entire body is in a state of deep sedation, which can increase inflammation and postoperative pain compared to local anesthesia,” McMahon said.
After the operation, Ralph’s pain medication was minimal, and he preferred to take less than recommended.
He used Advil for inflammation and could swap it out for Motrin if the pain level persisted.
Another patient, Indie (no last name given), spent 10 years addicted to heroin. She was in recovery for four years.
CLICK HERE TO SIGN UP FOR OUR HEALTH NEWSLETTER
When she suffered a burst appendix and was rushed to the ER in Houston, Texas, her sponsor shared her recovery status with the medical team and urged them not to give her any pain medications before the operation. Since it was an emergency, Indie was given a general anesthetic before surgery.
“After the procedure, her sponsor and family liaised with the medical team to keep her in the hospital for a few extra days,” McMahon said. “Barring any complications, patients can leave in one or two days, but this was extended to a week, so the hospital could monitor and manage Indie’s pain medication safely.”

“Patients with these complex issues may require additional care after surgery,” Dickerson explained. “A team of experts can plan and coordinate care that can help avoid a rocky surgical experience.” (iStock)
The pain medication was administered throughout a 24-span to temper the severity of the pain she was suffering.
“Self-administering of painkillers usually means the patient takes tablets when the pain starts to become unbearable, and this can then result in them looking elsewhere for stronger, more dangerous drugs,” McMahon explained.
“The use of around-the-clock dosing suppressed the pain and provided better comfort for Indie.”
Communication is key when managing pain in these complex patients, according to Dr. Lea McMahon, chief clinical officer at Symetria Recovery in Houston, Texas. (iStock)
Over the next seven days, the medication intervals remained the same, but the dose was gradually reduced.
After she was discharged, Indie was given a week’s supply of Tylenol and a non-opioid analgesic — and was instructed to call her physician twice a week to share her pain levels.
Above all, communication is key when managing pain in these complex patients, McMahon said.
“Advance notice to the health care providers will allow them to use alternative pain management strategies, such as non-opioid medications, physical therapy and complementary therapies,” she said.
“It’s a fine balance to strike, as too much can trigger the person in recovery, while not enough may have them looking elsewhere for relief.”
Read More: World News | Entertainment News | Celeb News
